We know you may have a lot of questions about the services we offer. We are happy to answer any questions in person, over the phone, or by email. But, in the meantime, here are answers to some common inquiries we receive.
If you have a question or concern that is not addressed here, just contact us. We’re always glad to help you.

What area of North Carolina does 3HC service?
3HC operates in eastern North Carolina, from the Triangle to the coast.
The counties included in our service area are below, with more to come soon:
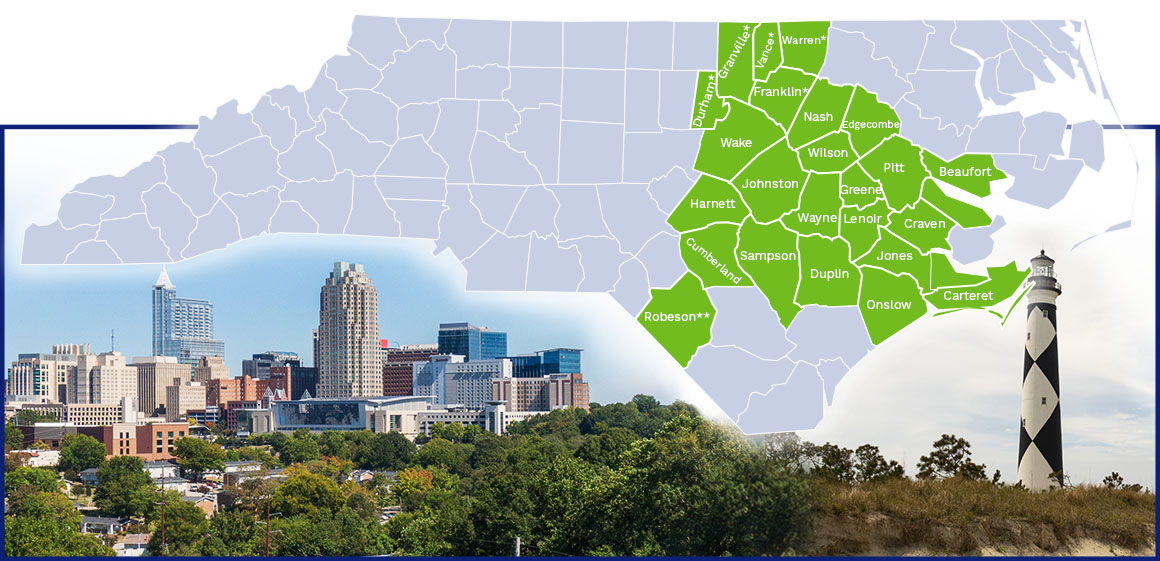
Beaufort
Carteret
Craven
Cumberland
Duplin
Durham*
Edgecombe
Franklin*
Granville*
Greene
Harnett
Johnston
Jones
Lenoir
Nash
Onslow
Pitt
Robeson**
Sampson
Vance*
Wake
Warren*
Wayne
Wilson
* Home Health Only
** Home Hospice Only
-
Yes, indeed. Home Health and Hospice Care, Inc, known as 3HC, has been around for over four decades. Our spread from one small office in Mount Olive, North Carolina in 1981, to now being one of the most respected hospice companies in the country proves our success.
-
Many hospice patients are eligible for the Medicare hospice benefit, which covers much of the cost. For those not eligible for Medicare, hospice care can be paid for through private insurance, and sometimes Medicaid. 3HC’s trained staff is knowledgeable about eligibility, coverage, and reimbursement requirements and will assist you with understanding your insurance benefits after verification.
-
In most parts of the country, over 99% of all home health services are paid by some third party/insurance company. All third-party payers have specific eligibility requirements and coverage parameters. Obviously, there are many specifics that relate to each third-party payer’s decision about a particular patient situation.
-
Many commercial or private insurance companies include home health benefits as part of their health insurance policies. In general, many commercial insurance policies require a prior hospital stay, physician’s orders, and need for intermittent skilled services to cover the cost of Home Health Services.
The number of visits, types of services and requirements for coverage vary greatly. Fortunately, 3HC’s trained staff is knowledgeable about eligibility, reimbursement, and coverage requirements and will assist you with understanding your insurance benefits after verification.
-
Approximately 80% of all home health visits are paid by Medicare.
In North Carolina, 10 – 15% of all home health visits are paid by the Medicaid program. Medicaid is primarily a state program designed to provide necessary health care to low-income citizens. Eligibility to receive services under the program is determined based on financial information, which is periodically reviewed.
-
To be eligible, a patient must have a physician’s statement confirming the terminal diagnosis with a prognosis of 6 months or less and must be in need of the comfort measures only (palliative care).
-
In Wayne County, the name Kitty Askins has become synonymous with comfort and care for a family’s most prized possession – loved ones on the threshold of their last days. The question of “Who is Kitty Askins?” always brings a smile to husband Richard Askins’ face, he says:
“People are curious what you have to do to have a building named after you. The truth is, she was just about the most normal person I have known – but maybe that’s the point. There are some people who can give without receiving. Are they extraordinary people, or regular folks, who accept our human responsibility to look after each other?”
Kitty pioneered home health services at Mount Olive, later to be 3HC, presenting the idea to local doctors and coordinating the process practically from the road, as she handled all the house calls. She was essentially the first hospice nurse in Wayne County and her compassion and commitment inspired all those around her. In death, as in life, one’s true legacy can live long afterward.
As her husband said, “Kitty’s story has no ending. It’s now just different people continuing the work.”
-
At the heart of home health and hospice care is the philosophy of retaining the patient’s dignity and comfort in their last days. The Dying Person’s Bill of Rights outlines the fundamentals of that philosophy in action. It was developed in 1975 in a workshop sponsored by the South Western Michigan Inservice Education Council, which was focused on needs of the terminally ill. It is as follows:
DYING PERSON’S BILL OF RIGHTS
- I have the right to be treated as a living human until I die.
- I have the right to maintain a sense of hopefulness, however changing its focus may be.
- I have the right to be cared for by those who can maintain a sense of hopefulness, however changing this may be.
- I have the right to express my feelings and emotions about my approaching death in my own way.
- I have the right to participate in decisions concerning my care.
- I have the right to expect continuing medical and nursing attention even though “cure” goals must be changed to “comfort” goals.
- I have the right to not die alone.
- I have the right to be free of pain.
- I have the right to have my questions answered honestly.
- I have the right to retain my individuality and not be judged for my decisions, which may be contrary to the belief of others.
- I have the right to expect that the sanctity of the human body will be respected after death.
- I have the right to be cared for by caring, sensitive, knowledgeable people who will attempt to understand my needs and will be able to gain some satisfaction in helping me face my death.
-
For your convenience, we have compiled this list of links below that will assist you in understanding end of life, hospice, and home health care. Please don’t hesitate to contact us with any other questions.
Helpful Links and Additional Resources
-
Official website for the Association of Home & Hospice Care of North Carolina (AHHC), a nonprofit association representing providers of home health, hospice, palliative care, personal care, private duty nursing, companion/sitter services, and more, with a mission to provide resources, education, advocacy, and leadership.
-
Official website for the ALS Association offering useful information about diagnosis and care of ALS patients, current research, resources and more.
-
Official website for the Alzheimer’s Association offering useful information about diagnosis and care of Alzheimer’s patients, current research, resources and more.
-
Website for the only organization in the United States for physicians dedicated to the advancement of hospice/palliative medicine, its practice, research and education.
-
Official website for the American Cancer Society providing information about cancer including diagnosis, support groups, research, resources and more.
-
CHAP’s mission is to provide leadership in enhancing the health and well-being of diverse communities achieved through the development of Standards of Excellence that assure the management of ethical, humane, and competent care in home, community, and public health settings.
-
As part of the Aging With Dignity Program, Five Wishes informs your family and loved ones of your intentions during the dying process or if you are unable to speak for yourself during a medical situation.
-
http://www.medicare.gov/HHCompare/home.asp
Medicare’s compiled listing of home care providers and their ratings compared to state and national averages. Searches are based on zip code, county, or state preference. In addition, searches can be completed by entering a particular agency’s name.
-
Professional site for nurses specializing in end-of-life care.
-
http://www.hospicepatients.org
Hospice patient advocacy site offering detailed information on hospice services, medical care, hospice selection, and more.
-
Shares hospice and palliative care information world-wide.
-
https://www.medicaid.gov/medicaid/benefits/hospice-benefits/index.html
Federal government offers a guideline for Medicaid recipients and details how one is covered for hospice care.
-
https://www.medicare.gov/coverage/hospice-care
Federal government offers a guideline for Medicare recipients and details how one is covered for hospice care.
-
NAHC is committed to representing the interests of the home care and hospice community.
-
The National Cancer Institute coordinates the National Cancer Program, which conducts and supports research, training, health information dissemination, and other programs with respect to the cause, diagnosis, prevention, and treatment of cancer, rehabilitation from cancer, and the continuing care of cancer patients and the families of cancer patients.
-
NHPCO is the largest nonprofit membership organization representing hospice and palliative care programs and professionals in the United States. The organization is committed to improving end of life care and expanding access to hospice care with the goal of profoundly enhancing quality of life for people dying in America and their loved ones.
-
The NC Dept. of Health and Human Services (DHHS) is the largest agency in state government, responsible for ensuring the health, safety and well-being of all North Carolinians, providing the human service needs for fragile populations like the mentally ill, deaf, blind and developmentally disabled, and helping poor North Carolinians achieve economic independence.
-
https://billmoyers.com/series/on-our-own-terms-moyers-on-dying/
An in-depth, thought-provoking site based on the four-part, six-hour PBS mini-series which aired in 2000. Issues include personal care, family response to terminal illness and death, the hospice philosophy and more.

